Projects
Accelerating innovation
Graduated Fellows continue working on the project proposals that came out of the program, mentored by Catalyst Europe Faculty. Fellows establish collaborations with international partners and institutions to cooperatively execute the research projects. They start and de-risk these projects to bring the innovation opportunities from an idea to implementation and impact in human healthcare. Project teams become agents of change.
PROJECTS
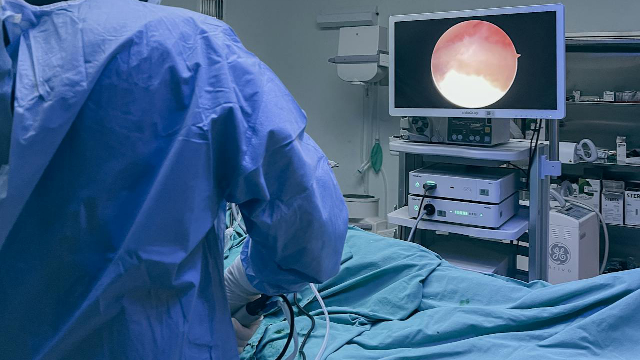
Ureteral Injuries
During endoscopic pelvic surgeries, high-energy (90+°C) instruments pose a significant risk of thermal injury to the ureters, especially in complex cases like endometriosis or advanced cancers. Current methods — such as dye injection or placing ureteral catheters for tactile localization — only assist in locating the ureter but do not prevent damage. This project proposes a smart ureteral catheter with integrated temperature sensors and an active cooling system. The device offers two key functions: early detection and alert of dangerous heat levels near the ureter and active temperature regulation to prevent injury. By enhancing intraoperative safety and injury-rate reduction, this solution has the potential damage to decrease postoperative complications, improve patient outcomes and lower healthcare costs related to injuries of complex surgical procedures.

ExoAnkle
Ankle sprains often lead to Chronic Ankle Instability (CAI), affecting 40% of patients and causing significant personal and economic burdens. Adherence is the main issue with current solutions for ankle sprains and Chronic Ankle Instability (CAI). Many patients struggle to consistently follow rehabilitation programs due to time constraints, discomfort, and inconvenience. Orthotic devices often prioritize reinjury protection but sacrifice comfort, leading to low usage. Without regular adherence to these treatments, recovery is delayed, and the risk of reinjury increases, perpetuating the cycle of instability and further complications. The project aims to address these challenges by integrating rehabilitation with a garment into daily activities, making it more convenient and comfortable for patients, thus improving adherence and overall outcomes.
Pacemaker
There is a recognized need for urgent access to pacemaker interrogation both in and out of hospital settings, often limited by compatibility issues. The project team is exploring triage solutions that could provide essential information about cardiac implantable electronic devices, thereby positively impacting their management. This project aims to address this unmet need by enhancing the efficiency and accessibility of pacemaker interrogation to improve patient care.
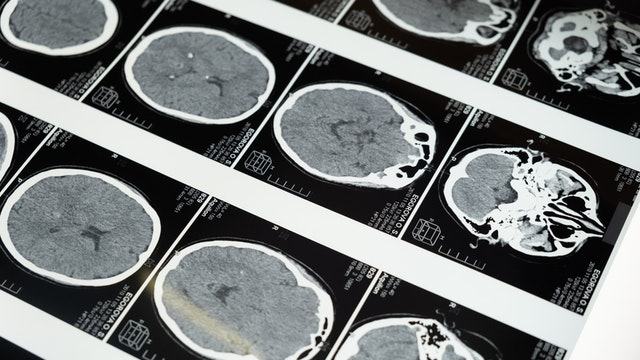
Improving Glioma Resection
Glioma is the most frequent and malignant brain cancer in adults. The first step of glioma treatment is tumor resection. To achieve maximum safe resection, neurosurgeons rely on intraoperative guidance for assessing which brain tissue can and should be removed. Current intraoperative guidance approaches are costly, time-consuming, and/or suffer from low sensitivity. This project proposes an optical approach for rapid, non-destructive and label-free intraoperative assessment of brain tissue to enable the surgeon to identify remaining tumor more accurately than existing methods. If successful, this approach will increase the surgeon’s ability to perform tumor resection, lower the risk of leaving behind safely-removable tumor and, thus, extend the time-to-recurrence and survival of patients.
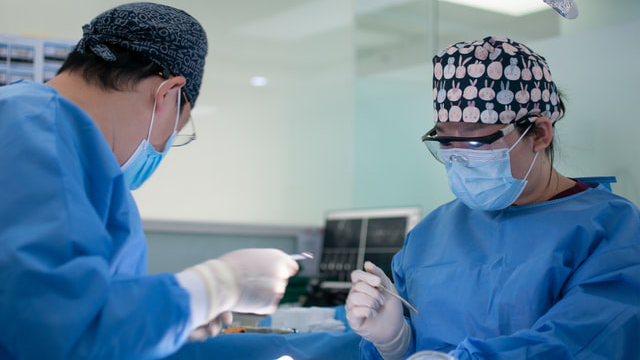
Surgescope
Surgescope has the mission to reduce the impact and outcomes of colorectal cancer in patients by harnessing free margins during tumor resection surgeries. Surgescope bridges augmented surgery and digital histopathology into a live intraoperative and collaborative suite. Through real-time observation of tumors with a fluorescence confocal laser endomicroscopy, Surgescope provides AI-powered decision-making tools for surgeons and pathologists to assess tumor markers and ensure free margins during surgery.

AIDAPt
Parkinson's Disease significantly impairs digital interaction due to motor and speech challenges, leading to decreased independence. Standard interfaces often fail to accommodate tremors or dysarthric speech, creating significant barriers to essential device use. AIDAPt addresses this by developing an AI-powered voice interface, aiming to provide a highly accurate PD-specific speech recognition model. This interface will enable individuals with moderate PD to reliably navigate smartphones and computers using voice commands, bypassing physical interaction difficulties. Our goal is to restore digital autonomy and improve quality of life by making technology accessible and independent for those affected by PD.

Period Poverty
Girls and women of reproductive age need adequate menstrual hygiene products for the management of their periods with dignity. However, the World Bank records that globally, about 500 million women and girls face limitations with access to menstrual hygiene products and toilet facilities in various communities. The high prices of sanitary pads coupled with limited washrooms in schools largely contribute to period poverty among girls from poor backgrounds. Consequently, the lack of access to menstrual management products and sanitary facilities promotes school absenteeism making it harder for young girls to get out of poverty. The project aims to address the difficulties with access to sanitary pads and other related matters that impede girls from attaining formal education in junior and senior high schools in deprived communities in Ghana by developing affordable, sustainable, and eco-friendly menstrual products thereby reducing school absenteeism and enhancing their education and livelihood for a better and brighter future.

An ultrasensitive screening test for malaria surveillance
Malaria has high mortality and morbidity in developing countries. Health authorities use epidemiological surveillance indicators to allocate resources to control malaria. A key indicator is the number of symptomatic and asymptomatic patients, as both sustain the transmission of parasites. These patients are identified using rapid diagnostic tests and microscopy, which fail to detect infections of less than 100 parasites/μl blood (typically asymptomatic). As a result, 30% of infections are missed and the prevalence of malaria is underestimated. This project wants to tackle this problem by developing a gold nanoparticle DNA sensor that is capable of detecting patients with low parasitemia. The test will be non-invasive and point-of-care, two features that make it optimal for surveillance campaigns.

Sneezalyzer
Bronchoalveolar lavage (BAL) is an invasive diagnostic procedure to identify community acquired pneumonia (CAP). Under conscious sedation it uses a flexible bronchoscope to collect fluid sample from deep lung regions for further examination. BAL has high diagnostic value, however, it entails discomfort, possible injury leading to painful breathing. There is a need for a low-risk sample acquisition tool that provides simple access to specimens allowing high-sensitivity CAP diagnosis. The project proposes sneeze as a lung-specific biomaterial with high amount of CAP-specific biomarkers, and Sneezalyzer, an innovative sampling device that induces sneezing and retains aerosol output. The non-invasive and pain-free solution offers high diagnostic potential with improved patient safety and experience.





